

autism awareness online home
About Our
Autism Site
about us
Articles on or about Autism
autism articles
Autism Information Webcast
autism webcast
Books on Autism
autism books
Autism Glossary
autism glossary
Autism Links
autism links
Autism Message Board
message board
Autism Resources: City, State, National, and International
autism resources
www.mommysangelinheaven.com
Guestbook: please sign that you have been here
guestbook
Search Engine
search engine
Site Map
site map

Rates and Packages
advertising
Banner Exchange
Banner Exchange
Paid Classifieds
autism classified ads
Plugboard
autism plugboard
Vote for Us: Topsites
Vote For Us: Top Sites
autism topsite
This is the story of how our beautiful baby girl Mariana became sick on July 1, 2008 and then passed away on July 16, 2008. It took only two weeks and two days for our perfectly healthy little girl to leave us for heaven and this is her story.
On Tuesday, July 1, 2008, I receive a call from Mari's summer school saying that she has diarrhea and needs to be picked up. I think they might be making too big of a deal over some diarrhea since we give Mari chocolate laxatives all the time. As a result, she can sometimes get diarrhea or loose stools. So I call Keith up and tell him he needs to go pick her up from school (since we only have one vehicle and he has it that day). He brings her home and she seems to be fine.
For the rest of the day she has several more episodes. Other than the episodes, she is completely herself, full of energy without any hint of slowing down. Keith and I talk that night about whether we should send her to school or not the next day. I know I want her to go to school so bad. She is going to have both July 3rd and 4th off due to 4th of July holiday. So, I really am not looking forward to having her home until Monday ALL THAT TIME. Just as a precaution, we decide to keep her home to make sure she is over her diarrhea.
ab cd ab
The following morning, Mari wakes up around 10am. I can hear her through the monitor playing and singing. It amazes me at how well she can entertain herself for so long. I know I should have gotten up right away to get her but I want to sleep in more. So I stay in bed until around 11am. She starts saying, “Let’s go potty” about every minute or so. Whether she really needs to go potty it does not matter because it is her way of letting us know she is done with whatever she is doing at that time. Usually, in the morning, it means she is up and ready to get out of her room.
So I get up out of bed and go down to get her out of her room. When I walk in I notice what either looks like diarrhea or throw up on her floor. Then looking further I notice it on her bed and smaller spots around her carpet. So I think, “Oh my poor baby girl!!” I decide that she needs a bath. I first get her all cleaned up and then put her in the bath tub. She just lays there with her head on her bath pillow. I decide to call Keith’s mom and have my morning chat with her.
Mari has been in the bathtub for about 10 to 15 minutes when she says in her always sweet sounding voice, “All done.” So I tell her just one second and go get her towel. I get the towel and tell Mari to stand up. She says again, “All done.” I say, “Ok Mari stand up.” She says ‘all done’ a couple of more times. I go to help her out the bathtub and it is like she cannot stand up. I tell mom that something is wrong with Mari and immediately get off the phone with her. I try to help her up by putting her hands on my arm. She becomes really wobbly and it kind of scares me a little. So I know she is not feeling good. I wrap her up in her towel and carry her to the couch in the family room. She just lays there all wrapped up. I go to get her some clothes to wear and then dry her off and get her dressed. Then I lay her on the couch.
Something I have not done since we moved on December 29th is to change Mari’s pediatrician. So I get on the phone with our insurance company and find a new one for her. I call up the new pediatrician’s office to see if we can get in that day since we have never been there before. The receptionist asks the doctor and she says we can come in as a walk in at 2pm.
When I get off the phone it is about 1:10pm. So I call Keith to come and pick us up as he has the van that day too. He gets there about 1:35pm. We immediately get Mari packed up and put her in the van. Keith decides to put a metal bowl in the van just in case. She hasn’t thrown up yet but you just never know. I leave the house at 1:40pm.
We make it to the doctor’s pavilion at Holy Cross Hospital around 2pm. I get out her stroller and take her out of the van. Then I put her in her stroller. I go back in the van to get her diaper bag and anything else we need. When I come back to her, she has thrown up all over herself. I quickly grab the metal bowl that Keith had put in the van just in case (which I am so thankful for).
So I take her up to the doctor’s waiting area and ask for a bathroom so I can get her cleaned up. We go in the bathroom. It is one of those single stall type bathrooms. I make sure to lock the door. I then proceed to undress her but I have no other clothes to dress her in. I have to call Keith to have him bring her a change of clothes. He is still at home waiting for a ride back to work. He is not happy as he knows we are going to have to make one of his recruiters drive him over to the hospital since he cannot get there himself. So he tells me he will ask and be over as quickly as he can. After I hang up, I wrap her up in her blanket so she is not just sitting there in her diaper.
We go out to the waiting area to be called back. Keith comes by about a half hour later with a top and a skirt. I think to myself, “Of all the changes of clothes he could have brought her, he brought a skirt.” So I take her back to the bathroom and get her dressed. We go back out to the waiting area and sit there until after 3:30 before we are finally called back. Once back in the office, the doctor examines her. She says that Mari is probably dehydrated and there is nothing she can do for her.
She tells me to take her down to the ER at Holy Cross Hospital. She will also call down to let them know we are on the way. I ask her if we are going to have to wait since she is calling and she says yes. Well, I am hoping that we can get in quicker because she is going to call. I mean, she is her doctor after all.
At this point, I call Keith and tell him what the doctor has said and we are heading downstairs to the ER. He tells me he will get there as soon as possible as he will have to get a ride. So we go downstairs and sign in. Keith arrives about a half hour later and we sit there taking care of Mari together.
The triage nurse finally calls us in to the triage office about an hour after we arrive at the ER. She says that the doctor has called, so they were expecting Mari. She goes on to say that when they have a room to put her in they will call her back to the ER. It seems like we wait forever. In the mean time, Mari starts to throw up about once an hour or more. At 6:30 I finally ask when we are going to be called back and I am told to talk to the charge nurse. She comes out and says that Mari was supposed to be the next one in but a person in respiratory distress just came in and took her spot. So I ask her how long she thinks it is going to take before she is called back. She says probably an hour.
So about 7:30 to 7:45pm time frame, we are finally called back. The moment Mari is being called back, she starts to throw up again. Keith is outside making a call and I cannot move. A really nice man helps me out by pushing Mari’s stroller while I hold the bowl as she is throwing up. We get back to her ER room and she has gone diarrhea again. The smell is so atrocious. I swear it can clean out a place. She then continues to throw up more and more frequently to the point of about every 5 to 10 minutes apart. She is just so sick.
Around 10pm, the ER doctor finally comes in and gives Keith and I a choice. He says that Holy Cross no longer has a Peds Unit at their hospital, so we can do either 1 of 2 things. Number one, we can take her home. If she does not seem to be improving or she gets worse, we should then take her to a hospital that has a peds unit. Or number two, we can transfer her to another hospital. My first instinct is to just transfer her for observation but Keith wants to take her home. I think it must have been my mother’s instinct clicking in to say let’s transfer her. But the way the doctor made it sound, it is really our choice and he is ok either way. Keith tells me to go and talk to the doctor because he would prefer to take her home. So I do. The doctor basically says that if they had a peds unit he would admit her to their hospital but they don’t. So he leaves it up to us, but I think just the way he talked he would prefer her to be transferred. So I go and tell Keith and we decide to transfer her.
I ride in the ambulance with her and sit in the front seat. About half way to Stroger Hospital (formally called Cook County Hospital) there is this very foul smell. I ask if that is her or is that coming from outside. The paramedic in the back says it is her. The ambulance does not go by lights and sirens to the hospital. When we get there we go to the pediatric ER and they immediately take her in the back to a bed. We clean up her diarrhea. She has another episode of diarrhea. This is the second one we change at Cook County. When I change her third one, I start to notice what looks like red that may have been blood but the nurse does not say anything. She has a fourth one and still the red again.
We finally get a room upstairs on the pediatric floor. She has a fifth one and the nurse from the floor this time notices the red too. She says it looks like blood and I tell her I agree. I tell her I did not say anything downstairs in the ER but the nurse down there did not say anything either. The nurse tells Keith and me that this is no longer a viral infection but instead it is a bacterial infection due to the blood. This obviously becomes a concern. With this diaper, we are trying to change it but it is like we cannot get it changed quickly enough. We don’t even have a chance to close it up before she has another episode. She has three just bam bam bam. She continues to have diarrhea throughout the night. When she was at Holy Cross Hospital, the doctor had given her something for her nausea and throwing up, so she is not throwing up during this time. Also, only one parent is allowed to stay in the room at night with her. So, Keith goes home as there is no way I am leaving her side and Keith truly hates hospitals.
ab cd ab
The next day is mostly Mari just sitting in bed with diaper after diaper of diarrhea. The doctors tell us today they are 90% positive that Mari has Shigella (probably misspelled). It is caused by E. coli. This is about 11 o’clock in the morning and they are going to start her on antibiotics to fight the Shigella.
In the mean time, I call Keith’s mom and tell her that Mari has been admitted to the hospital. She figures Mari will be home in a day or two and will come over to visit her then.
The antibiotics are finally given to Mari via IV at 7pm that night (You think it took them long enough J). She starts to throw up in the evening. Throughout the night she continues to have more diarrhea and throwing up.
ab cd ab
On Friday, July 4th, Mari seems to be slowly getting worse. She seems to now have the shakes all over her body. When she tries to pick out a DVD to watch her hand is shaking so badly. She still has continuous diarrhea and throwing up. She now has not eaten since Tuesday, July 1. She gets her second 24 hour dose of antibiotic at 7pm. It seems like Mari might be getting a little bit better only because for the first time since getting sick she actually sleeps for a good 6 to 7 hours straight. At this point I am really starting to notice that she is not peeing very often. The last time she had peed was about 12 noon and maybe 12 to 18 hours before that. The doctors just keep saying its ok because she has been having so much diarrhea. They say the fluid she is losing in her diarrhea is causing her not to go pee that often. I am now also starting to notice that she is starting to somewhat swell up but not too terrible. At the beginning of the day the doctor tell us her platelet count is also starting to fall. She had been at 100,000 the day before and now she is at 80,000.
Because today is the 4th of July, Keith and I are able to watch the fireworks from the hospital room window. We thought we were going to miss it. It is kind of nice to know we can at least see them. Keith heads home around 1am and I stay with Mari again. I just push her over a little bit so I can lie beside her and cuddle next to her for the night. I guess you can say I just need to feel close to her.
ab cd ab
The next morning I wake up around 7am and I notice
that Mari’s face on her right side is so swollen that her eye is almost
swollen shut and her left arm, with the IV in it, is very badly swollen
as well. I ask the nurse to
check it and she says that it is fine.
When the attending physician and the residents go on rounds they
come in and tell me that Mari no longer has Shigella but instead she has
E. coli and the strand she has is O157:H7 (To read more about E. coli
O157:H7
http://www.cfsan.fda.gov/~mow/chap15.html).
They say that they are immediately stopping all antibiotics as
they make this in particular E. coli worse.
As a precautionary measure, she is having her transferred over to
the Pediatric ICU just for observation.
She also tells the nurse to take out the IV and start her it
someplace else with how swollen her arm is.
I start to cry because people do not get transferred to ICU for
something as simple as her diarrhea.
At this point she still has not peed and they cannot tell me it’s
because of her diarrhea as all people have to go pee to get the
pollutants out of their body.
So I call my husband Keith to let him know. Then I call his mom as well. Keith finally arrives around 9am. In the mean time, the doctor has the nurse relocate her IV because of the swelling. They bring in 3 or 4 other people as well because I tell them Mari will fight tooth and nail against another stick. Mari starts to fight and squirm. It is hard to hold her down. Then her nurse that is assigned to her for that shift actually tells Mari, “Now, don’t you want to get better. You need to sit still so we can do this.” I look at her and say in the nicest way I can possibly muster, “She has autism and doesn’t understand.” She says, “She does. I did not know that.” That does not bode well with me at all. She should have been told during the shift change from the previous nurse. Better yet, I know it is in her chart so that just tells me she did not read up on my daughter at all, at least not very thoroughly. Keith’s mom and sister Amy arrive around 10am. We get everything ready to go for the transfer.
I have not taken a shower since June 30th as I was going to take one on July 2 but Mari became to sick so I never get around to it. We ask the nursing staff if she is being transferred anytime soon. They say no. So I hop in the shower around 10:30. Boy that felt like one of the best showers I have had in a long time.
When I get out, get dressed, and go back into her room, Keith’s mom tells me they had come to transfer her while I was in the shower. I am like, “Of course they did.” So I quickly pack up all my toiletries and what not. Then I go and get the nurse to tell her we are ready to go.
Mari gets transferred to the ICU around 11am. When we get to the ICU, they decide to give her a folly catheter to see how much urine she has in her bladder. I hold her arms, a nurse holds one leg, and another nurse holds the other. She screams bloody murder at the top of her lungs and fights so hard so we will stop. The doctor then tells us that they may need to transfer her to UIC (University of Illinois Medical Center at Chicago) to start her on dialysis because her Kidneys are failing.
Before they are going to transfer her they want to try a couple of different medications to force her to go pee. While we are waiting, Amy decides to take me to the grocery store so I can get some food to eat. I have not left Mari’s side other than to go to the bathroom or get a nurse. So everyone thinks it will be a good idea to give me a break.
At first we stop at Subway so I can eat something besides hospital food. Boy did that taste good. Then we head over to Jewel/Osco. I get a lot of snacks and different things to eat for meals. We are gone for about 45 minutes to an hour then head back to the hospital.
About an hour after we arrive back, the doctor tells us the medications have not worked. So ultimately she needs to be transferred to UIC. They also tell us that her morning platelet count was at 65,000. So it has dropped another 15,000 from the day before.
She gets transferred to UIC around 2pm (I think) and the attending physician tell us that they are not actually going to start dialysis but instead they are going to push about 4 to 5 different types of industrial strength diuretics down her to get her to go pee. With everything they push down her, she only pees 23 milliliters. Her platelet count drops down to 58,000 from just five hours before. Four hours later, the count drops to 26,000. Four hours after that it drops down to 25,000. This is not looking good at all.
It is as if she is slipping further and further down right before our eyes. She seems to be getting less and less responsive as the day goes on. She sleeps most of the time now. About 1am I am concerned because it seems like she is not being responsive at all. The doctor comes in and checks her. It takes a bit to get her to respond him. This scares me at first because the doctor keeps talking about how there could be “brain issues”. So anytime I think she is not being responsive enough, I have the doctor check her.
She still has some fight in her and is making it hard for the doctor to examine her. She makes it hard to check her pupils. I try to sooth her by saying her name. She actually repeats back to me and says, “Mari.” She doesn’t want her arm touched so she tries to fight that as well. After the doctor is done checking her I feel relieved to know that she still seems to recognize us and is still fighting.
Around 2am the doctor comes in and talks to me about needing to sign paperwork. It is just in case they have to perform any emergency procedures on Mari. I think I am sort of in a fog at this point because her condition has deteriorated so quickly.
I do not want to make any decisions on my own and Keith went home around midnight. So I decide to call him. I put him on speaker so the doctor can go over some of the procedures that may need to be performed before morning. Some of them include putting in the dialysis catheter, a central line, and giving her either a blood or platelet transfusion. We agree to any procedure that will help her and I sign the paperwork.
Through all of this, Mari’s nurse keeps telling me I need to go to sleep as I will not be any good to her if I do not. I finally lie down and do the best I can considering the situation. As you can imagine, it is not very much or very good. I wake up several times throughout the rest of the night.
ab cd ab
I get up the next morning around 9am. The first thing I do is to check on Mari. She doesn’t seem to be awake or responsive. I try to wake her up but can’t. I go get the doctor and he comes in to examine her. He can’t get her to respond either. Now, it seems her left side is not moving and he’s not getting any reflexes. It seems like both the left leg and left arm take forever to even get a little bit of response.
The doctor then pulls me aside and asks me, “Do you remember me talking about Mari having possible brain issues?” and I say, “Yes.” He goes on to inform me that the “brain issues” he was talking about was a stroke and it looks like Mari may have had one. I just break down. I cannot believe this. What seemed like a simple case of diarrhea has turned into kidney failure and now a possible stroke. He says she needs to have a CT scan performed and then maybe an MRI to find out for sure.
I call Keith and tell him what I have just been told. We are both just so devastated. He heads up to the hospital immediately. I also call Keith’s mom and dad and tell them as well. They were already planning on coming up to the hospital that morning anyway.
Once Keith arrives at the hospital, he stays in the room and waits for his mom and dad. I go with Mari to get her CT scan. They allow me to stay in the room with her while they perform it. After the scan is completed, I stand there holding Mari’s hand while the doctor and other people take a look at her scans. There is a long window to where you can see everyone looking at the one monitor for the scan they just took and discussing something. It seems like we wait forever before the doctor finally comes in the room and says we can head over to where the MRI will be performed. He will be right behind us but has to go and do something really quick.
So I am now in the MRI area helping Mari get on the MRI cart. I take off all my metal objects (like my earrings, watch and other items) and fill out a form so I can be in there with her. I am cleared to come in the room. I am helping the nurse when the doctor comes back. Both the doctor and the nurse decide to stay in the room with her. Then the doctor tells me the CT scan looks very suspect that she indeed had a stoke but the MRI should be able to confirm it. I just simply break down. I cannot believe it. I cannot even stay in the room and tell them I just need to go back. I need to go and talk to Keith. So they have this woman walk me back to Mari’s hospital room. I get back to the room and Keith’s mom and dad are now waiting in there for us to come back. I walk in and they can tell right away that something is wrong. I tell them what the doctor has told me and we are all in utter disbelief.
The doctor finally comes back with Mari (it seems like we wait forever but it only takes about 20 minutes). He then takes all of us to a consultation room along with the Kidney doctor to let us know what the results have found. He lets us know that it was definitely a stroke. He then goes on to say that both pediatric neurologist at UIC retired on July 1st and he cannot in good conscience keep Mari at his hospital. He feels she needs to be transferred, yet one more time, to Children’s Memorial Hospital. This will be her 4th hospital in 5 days.
The transport services arrive about a half hour after the call is put in to have her transferred. They have two paramedics and two RNs with this service. The doctor tells me if we had to wait 3 to 4 hours he would have gotten the dialysis catheter in immediately so dialysis could have been started as soon as she was transferred.
When we get to Children’s Memorial there are more doctors and nurses waiting for us than I think I have seen to admit one little girl. It is kind of reassuring to know that there are that many people. We are not at the hospital for more than an hour when they take her off to go and put in the dialysis catheter and the central line because they want to immediately start her on dialysis. She is so swollen by now that to feel and look at her skin it is just so tight and puffy. They come back and start her on dialysis within about 3 hours after arriving at the hospital.
The rest of the day seems pretty calm, all things considered. We have family come to see her and we really thought we were going to lose her this day. She makes it through the night and her platelet count seems to finally come up around the 40,000’s. They seem to have stabilized. Mari’s nurse from that night tells me about the Ronald McDonald House and to ask to speak with the Social Worker the next morning about getting us a room there.
ab cd ab
Today is Monday, July 7th and it is a pretty calm day. Mari stays on Dialysis. She seems to wake up here and there but she is unresponsive. We ask the neurologist several things but basically it is all about patience and a wait and see game so to speak. She remains on the 24/7 dialysis. She is still very swollen.
I talk to the social worker that morning about seeing if we can get a room at the Ronald McDonald House. She says sure. She calls over there and get us on the waiting list. We do not get a call that day for a place and are told to call again the next day to see if a spot has become available. She now has not had any diarrhea since late Saturday night.
ab cd ab
The next day, Mari is starting to stay awake more and more but she is still completely unresponsive. It is like the lights are out. She remains on the 24/7 dialysis and seems to be inch worming slowly but surely in a positive manner. No real change happens today. She still has had no diarrhea since Saturday.
I call the Ronald McDonald house about 11am to see if there is a spot for us yet. They say no but they will call me if one comes open or to call back again in the morning to see. They call about 2 or 3pm that afternoon to let us know there is a spot for us. So, Keith and I walk over to the house, sign in, get our room keys, receive a tour of the place and then walk back to the hospital. Keith does not have his stuff here yet so we do not use the room that night.
ab cd ab
On Wednesday, Mari is even more awake now. She woke up about 3pm and did not go to sleep again for the rest of the day or night. She is still on 24/7 dialysis. She seems to be less swollen as it has gone down quite significantly. Other than that there are no real changes and she is still unresponsive but awake.
Keith brings his and my stuff. We decide to leave for a while and we go to Target. I buy Mari’s “take me home from the hospital” outfit to hang up in her room to see all the time. I buy her the “Happy Feet” DVD and 2 Wonder Pets DVDs. “Happy Feet” is one of her very favorites and she simply loves the Wonder Pets. We get some groceries and I pick up a couple of hand held games. We go back to the Ronald McDonald house to drop off our stuff. We eat dinner and then head back to the hospital. Keith is now close by every night. It is nice that he does not have to go back and forth and he is only about a 5 to 10 minute walk away.
ab cd ab
It’s hard to believe that Mari has been in the hospital a little over a week. She remains awake for the rest of the day. At one point when we think she is finally going to sleep, she closes her eyes for about 5 minutes and then wakes back up for the rest of the day. The Attending at the beginning of the day is a little concerned and just wants to watch that. She also seems to be getting more concerned with the fact that she is still unresponsive. It is just like the lights are out and completely gone.
Keith and I remain at the hospital for the rest of the day until it is time to go to dinner at the Ronald McDonald house. They have different groups of people that come in either for lunch or dinner or even both each day to cook food for those that are in the house. We think dinner is at 5:30pm so we head out about 5:15pm. I am finally getting to the point where I am feeling comfortable enough to leave Mari alone for small periods of time. So Keith and I walk over together.
We get to the house and find out that we are an hour early and dinner is not going to be ready until 6:30pm. So we just hang around and watch some TV (I believe we get sucked into watching “The Sandlot”) when Keith gets a call on his cell phone about 6:10pm from the hospital telling us that Mari had a seizure while we were gone. So Keith and I head back upstairs to see if we can eat early. We quickly eat right at 6:30pm then go back to the hospital.
When we get back to the hospital we find out that her seizure lasted about 10 minutes. At first they were not going to do a CT scan and then all of a sudden we have to get one right away. They take her off of dialysis and go to get her scan done.
By now we have called Keith’s mom and dad. They are on their way to Keith’s sister Amanda’s music concert with a close family friend Gina. They decide to head up to the hospital instead. Keith and I know that it must be quite urgent for the doctors to change their mind that quickly from not needing a CT scan to now needing one.
Mari comes back from her scan and they tell us they had to give her a seizure medication to stop the seizure from before and then an anti-seizure medication to prevent future ones. Then around 9 or 10pm Mari starts to do this posturing. Then she seems to be having a hard time breathing and the sound is very strange but this only lasts about 20 to 30 seconds. Then she stops for 20 to 30 seconds. Then she starts again. This goes on for a good 30 minutes.
The doctors are paged and we now find out these are continuous on and off seizures. So this last 30 minutes is really not a good thing. She is now also biting down on her tongue. They give her more Adavant (the medicine to stop seizures in progress) and the anti-seizure medication to prevent future ones. Now she is going to get them on a constant basis.
Because they don’t want her tongue to block her airway, they go ahead for preventative reasons, decide to intubate her and put her on a ventilator (or a breathing machine). Keith and I are fine and understand that. To be quite honest, we all thought we had already crossed this bridge to where she was not going to have seizures and she would not need to be intubated. The rest of the night is pretty uneventful. Keith leaves for the house around 11:30pm. I go to sleep the best I can.
ab cd ab
I ask the nurse from the night before to make sure that I am woken up as soon as the Neurologist comes in because I want to talk with him. The next morning she wakes me up around 7:30am. Right at 7:40, the Neurologist checks Mari’s pupils and they are still reactive and small. I am able to ask a few questions like why she had a seizure. He says because her brain has been so severely injured that the injuries may be causing them. I understand that and remain awake for the rest of the time.
Right at 9am, the radiology team calls the doctor to say there is something that looks suspicious on her CT scan from the night before and right about the same time Mari’s pupils look like they have exploded. There is basically no color left to her eye. I am told at one point that her pupils even look kidney shaped. The attending then tells me that she has called neurosurgery to come in and check Mari because she may need a procedure done. I call Keith to tell him to get over to the hospital immediately. Then I call Keith’s mom to inform her about what is going on. Mom calls Keith’s dad and she heads up to the hospital with Gina.
In the mean time, the room just seems to be getting busier and busier with more and more people. Then a chaplain by the name of Jim comes in and starts to talk to me. He says they call the chaplain in when the parents might need the support. I ask the PICU Attending if this procedure they are preparing for has to definitely be performed on Mari. She says 100% it has to be done because Mari has so much cranial pressure building up due to her brain swelling. If they do not go into relieve the pressure, she will die. The neurosurgery team needs to go in and put a shunt in to relieve the pressure. Obviously I do not object and say let’s do it.
The Attending Neuro Surgeon talks to me about what needs to be done. He says that first they are going to take her down for a quick 5 minute CT scan and then head to the OR to perform the procedure to put the shunt in her head. I sign the necessary paperwork to allow them to perform the procedure. Keith arrives about 15 to 20 minutes later.
We are talking to the chaplain telling him about Mari when all of a sudden in the background you hear someone yell, “We need a crash cart. She is coding.” Needless to say, Keith and I are just a little freaked out. They quickly rush us out of her room into the hallway. I fall to a heap on the floor just hysterically crying. They get both Keith and I a chair to sit on. The social worker is here by now as well. I keep asking the social worker if they are still performing chest compressions and she says yes.
It seems like time just stands still. It feels like the compressions last at least 15 to 20 minutes. During all of this, Keith’s dad arrives at her room. They are still performing compressions on her while performing an emergency procedure at her bedside to put the shunt in.
For the first time Keith cannot be the strong one for both of us anymore. He has his first crying break down because the seriousness of the situation is so overwhelming, and the fact that we just might lose our daughter is just too much to take for the both of us. It seems like all of our hope gets smashed in one split second. The neurosurgery team gets the shunt in and Mari’s heart rate comes back up to where it is supposed to be.
The next thing we are told is that they are now going to take her to get a CT scan and then they will be back in 20 to 30 minutes. They bring her back and now it seems like it is just a waiting game. The whole family arrives one by one to give us support. Keith and I really thought we were going to lose her. We are in complete disbelief with what we just witnessed with Mari. I saw Keith cry and break down for the first time because we actually thought we were going to lose her.
The social worker and the chaplain reserve a special waiting area for us so we do not have to be around others in this time of crisis. It is so reassuring and comforting to know that our family, which includes Keith’s Mom and Dad, Keith’s sisters Amanda and her husband David, Peggy and her husband David, Amy and Becky, and a close personal family friend Gina and her daughter Danielle are there to support us and comfort each other.
The afternoon seems to be such a waiting game to see how things will go and it seems like Mari has at least stabilized considering the situation that happened this morning. We always have at least 1 to 2 people in the room with her at all times.
They immediately put Mari back on dialysis. Keith comes in about 2pm and says that the neurologist just talked with him and said that the CT scan shows the affected area from the stroke has gotten bigger from the night before. Amanda and I then decide to go back to Mari’s room to go visit with her. I see the Neurologist down the hall from Mari’s room and decide to hear for myself exactly what he had said and to also ask my own questions. He tells me that it has gotten bigger; they want to do a new CT scan the next day and then go from there. I say ok and then head back to Mari’s room.
I walk in her room and the nurse says that the shunt has quit working and they are talking about taking her back for another CT scan now. They have just restarted the 24/7 dialysis and I know starting and stop her dialysis is not good. It can cause so much uncertainty in her body and cause problems doing this. The nurse gets a call that they definitely want to take Mari back for another scan since the shunt has quit draining. She says they know the line is not clogged and they need to see what is now going on. So they take her back off dialysis yet once again.
Amanda and I go back in the waiting room where the family is. We tell them what just happened and how the Neurologist had just told me one thing and just that quickly they have changed their minds. Keith’s dad is actually ready to head back home and decides he better stay now. We are all very nervous about this new development.
They take Mari off to CT. We all wait for her to come back. As soon as she is back, Keith and I head back to her room to wait for them to come and tell us. One of the Neurosurgeon Fellows comes to talk to us and asks if we want to see all 4 of her CT scans. We all say yes. So Keith, Becky, Dad and I all follow the Neurosurgeon to a computer to show us. He then decides to show us a random child’s CT scan to show us what a “normal” brain looks like. He then shows certain things of the scan to explain what looks normal. He then brings up all 4 of Mari’s scans on the computer at the same time.
First, He shows us Mari’s first scan after the stroke from Sunday. He shows us exactly where the stroke has taken place (which is around 2 inches in diameter). He then shows us the scan from last night (Saturday) and how much it has grown (which now looks to be about 4 inches in diameter). He then shows us the scan from about 12 hours later, the first one done today after all the trauma from earlier. It shows that it has grown even bigger. By the 4th and final scan it looks like the stroke covers the entire brain and that is what he says it looks like. We are all just completely devastated. I know right then and there that she is probably not going to make it by that scan. I just break down crying. We go to inform the family what was just shown to us.
Around 8pm, the attending physician lets us know that the team (which consists of the attending physicians for PICU, Kidney, Neurology, Neurosurgery, PICU Fellow, and our nurse) wants to have a talk with us as to what they believe and what they have seen. So we get Mom and Dad, and the four of us follow the team into a meeting type conference room. We all sit around a big table to discuss what they found. Well I like to call the meeting the “Doom and Gloom Round Table Discussion.” They have almost nothing positive to say. They all tell us that she probably will not survive the night. They feel she is going to become brain dead by morning. They go on to say that we should get a hold of anyone who would want to say goodbye to Mari as they need to get here that evening or no later than the next morning. They feel if she does not go brain dead that she has a very slim chance of ever doing anything again for the rest of her life. We are all just so devastated. The Kidney doctor says it is pointless at this point to start her back up on dialysis unless she makes it through.
So basically it is time to call all of our friends and family in the area to let them know that if they want to come and say goodbye to Mari they need to do so that night or first thing in the morning because we are more than likely going to lose her by the next day. I personally don’t think I have made more difficult calls in my life before. Everyone is completely and utterly shocked and disappointed because no one expected this to happen.
Our nurse and the other medical personnel all make an exception for us with the amount of visitors we can have and actually get more chairs for us as we are technically only aloud 3 visitors in the room at a time. Mari’s night nurse is named Cindy. She is exactly who we need this in particular night. So God does do things in such mysterious ways. She is just so understanding.
We have all of Keith’s recruiters that he is in charge of and their spouses come up, several of our friends from DeKalb come to visit (which is a good hour and a half to two hours away and it is where we moved from back on December 29, Mari’s 8th birthday), all the family is there minus a couple of Keith’s brothers because they are too young, and some of our Army Family also comes to say goodbye.
Keith has a couple of breakdowns because it just seems so daunting and unbelievable that we are going to lose our daughter. We just hold each other because we love each other so much and are just there for each other. I could not have a better husband than Keith. God knows he is perfect for me.
The final people leave around 1:30 to 1:45 in the morning. Keith’s sister Becky stays the night with us in the room. Cindy (the nurse) gets another one of the chairs that fold out into a bed for her. She moves Mari over in her bed and allows me to sleep beside her for the night.
Once everyone leaves, Keith and I are no longer crying and we are able to talk about the DNR (Do Not Resuscitate Order) we want for Mari because it seems inevitable what the outcome for her is going to be. We have decided that we just cannot do anything. We both agree that ABSOLUTELY under no circumstances will they shock Mari but we do want them to push meds and do chest compressions with her. We also have come to an agreement that if Mari were to stay in the state she is in now that we will decide to remove life support when the time is right. This has been a hard decision for us but we know it is the right one because the Mari we all know and love no longer exists at this point and it will just be selfish on our part to keep her alive this way. We love her too much to ever do that.
The Army also seems to amaze me all the time. During our time of need they have flown out the Brigade Chaplain to be there just for us. This has impressed me more than they will ever know. It is just so comforting to have him here. He arrives around 9pm. We thank the Army so much.
Our day never seems to end but eventually we all go to sleep for the night (or at least we tried).
ab cd ab
Saturday seems to be the day after the storm for us. Mari has her first visitor arrive at 8am. Throughout the rest of the day, she has a steady flow of visitors. Sometimes there are quite a few at one time.
The Attending talks to us that morning and tells everyone who happens to be in her room, that Mari’s last CT scan is the worst CT scan she has ever seen. Not only did she say that once but she says it twice in the same conversation. Needless to say, no one is happy to hear that.
Well, they do another EEG that lasts about an hour. When I look at the brain waves it seem like the EEG today is much better than yesterday’s. I think we are going to get a positive report as the one from yesterday did not look good at all. When the neurologist comes in he tells us there really is no change from the day before. I tell him what I have seen and I want to know how it has not improved because it looks like it was better. He says that the sensitivity was probably at a higher setting so it looked better than it really was. I am simply crushed as I let my hopes get way too high. I completely break down. All those in the room, and there are quite a few at this time, feel totally devastated. It is like we have this balloon that was filled with air to maximum capacity and suddenly becomes deflated all at once. Everyone can feel the balloon deflate and there does not seem to be a dry eye in her room as almost everyone is crying. My father-in-law is trying to talk about children in the Bible and for the first time he breaks down crying. Bottom line, I think everyone is just devastated.
I ultimately have a meltdown to where I just cannot function anymore and cannot even answer simple questions that are being asked of me. So the nurse asks me if I would like to take a nap beside Mari. I say yes. She moves Mari over. The nurse and Keith clear out the room so I can just sleep for a little while. My best friend Shelly stays with me and just rubs my back until I am practically asleep. That is one of the most reassuring and comforting things for me. I fall asleep pretty quickly. My husband says I slept for at least an hour and half but no more than two hours. When I wake up, everyone is gone except my sister-in-law Amy because she is staying over with us. The family wants to make sure we have at least one family member with us at all times during this time which we are very grateful for.
We all go to the Ronald McDonald House around 5:30pm for dinner because there is supposed to be a group of people to come in and cook dinner for everyone in the house. Well, they never show up. So we scrounged around and eat leftovers. I then take a shower which helps me to feel so good. We go back to the hospital and I am pretty numb for the rest of the night. I am just trying to take everything in.
At some point during the early evening, Mari’s shunt starts to drain again. This is such a good sign as it means the swelling in her brain is starting to decrease. You can see blood in the drainage tube. They tell us this is normal. It is such a major relief for all of us there.
The Attending PICU tells us that they want to take Mari for a MRI first thing in the morning. We ask her why since we are told that to get a really good MRI you need to wait about 7 days after the injury takes place. She tells us it is to help us with our decision making process. The reality of everything that has happened just seems to get to be so much sometimes.
Amy and I go back to the Ronald McDonald House around 10:30pm to go to sleep that night and Keith stays behind with Mari. I go to sleep around 12:15am and for the first time I sleep straight through until I receive a phone call at 7:45am. It is the best night’s sleep I have had since Mari went in the hospital almost two weeks ago Wednesday.
ab cd ab
Amy and I get up around 8am. We are back at the hospital around nine. By the time we get to the hospital they have already taken Mari to the MRI (which lasted at least an hour if not more) and returned. It seems like for the rest of the day we just keep waiting for Neurology to come in and let us know what they found.
In the mean time, Keith’s Battalion Command Sergeant Major (CSM) Thorpe, his wife Jennifer, and their son Chance, and his Battalion Commander Lieutenant Colonel (LTC) Box, his wife Kathy, and their son and daughter come for a visit. It is really nice that they came to see how Mari is doing.
We all decide to go out to the waiting room and tell the nurse that when they are ready to talk to us we will be in there. I get a call on my cell phone saying they are ready to come and do the round robin again with us. We do it right in the waiting room. The CSM, the LTC and their wives and children all go into the hallway while they come in to tell us what they found. Amy and the Army Chaplain are still there with us.
The doctors that are there is the Attending PICU, the Fellow PICU, and the Attending Neurologist. What they say to us is that the MRI is pretty bad but it does not show that the stroke has covered the entire brain. The MRI confirms what her initial CT scan showed in that her stroke is in the middle of her brain. They now believe she will not become brain dead so long as no other complications arise. Now it is just a wait and see game. They also talk about her brain stem and are unsure how injured it had become on Friday. The MRI does not show any injury but they can tell she did due to some of the exams they have done on her and how she is not regulating her own body temperature. They also talk about how they would like to start weaning Mari off the ventilator to see if she can start to breathe on her own.
We go out and tell the others what has been told to us. Everyone is very happy to hear the news. It feels like the first piece of real good news in quite some time.
The rest of the day is pretty calm. Everyone eventually leaves. Keith and I decide to start alternating each night with one staying the night in the room with Mari and the other going to the Ronald McDonald House so that one of us can get at least one night of good sleep every other day. Because I stayed the previous night at the Ronald McDonald House it is Keith’s turn.
The rest of the night is pretty calm.
ab cd ab
Today seems to start off as a pretty calm day. The Neurologist comes in and talks about her MRI. He says that the MRI shows the stroke did not cover the entire brain like they had thought but it does show that the stroke is pretty hard hit in the middle of the brain. He does say that Mari is now back to where she was on Thursday. We are so happy to hear that. He says that it is completely a wait and see game with her. He also reiterates what they told us yesterday in that they are not sure how much of her brain stem became injured during the ordeal on Friday. They know that it has been but the MRI does not show it being injured. However, they can just tell by their exams of her. We are all very happy with this news.
Then the Nephrologist (kidney doctor) comes in to just confirm what we already suspected in that Mari’s kidneys have a very slim to no chance of ever working again. They need to do an ultra sound to see if there is still any blood flow to them to find out. If there is no more blood flow to her kidneys, she will have permanent loss of them. Until Mari’s neurological issues improve quite a bit she will not be a candidate for a kidney transplant. This makes sense of course in that there is no reason to give someone a kidney transplant if they are not responsive.
The Hematologist comes in and does not give us a straight answer as to whether she has HUS or TTP for sure. I think it is because they really do not know. She says that they are just going to continue with the course of action they are doing now since this is what seems to be working.
The starting of the day, Mari’s pulse is at about the 100’s which is very good. When the Attending PICU does her rounds she talks about and decides that they will try to start weaning Mari off the ventilator during the day. We are happy to hear that. So they first drop her from sixteen respirations per minute down to fourteen. What we start to notice as the day goes on is that her heart rate starts to level out in the 90s and then in the 80s. Later in the day they drop her down to twelve respirations per minute. Then you start to see her heart rate dropping down into the 70s, and finally into the 60s, with it sometimes even dropping into the 50s (which is really not good). Keith and I are getting pretty concerned. Since her respiration amount is the only thing that has changed, we concluded that she is not doing so well on the lower respirations. Eventually the doctors feel the same way and they put her back up to sixteen respirations per minute. Her heart rate seems to go back up with the fast breaths. We are happy. They keep her like that for the rest of the night.
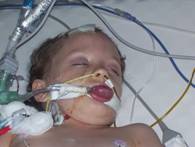 Now
Mari’s tongue has become pretty bad at this point.
In fact, her nurse says that in the last 5 years she has worked
here she has never seen a tongue like this before.
They have to bring in a dentist to try to get a bite block in
because Mari is biting down so hard on her tongue that it just keeps
getting bigger and bigger and more and more discolored.
It just looks like it hurts.
Now
Mari’s tongue has become pretty bad at this point.
In fact, her nurse says that in the last 5 years she has worked
here she has never seen a tongue like this before.
They have to bring in a dentist to try to get a bite block in
because Mari is biting down so hard on her tongue that it just keeps
getting bigger and bigger and more and more discolored.
It just looks like it hurts.
The dentist puts in this metal contraption in her mouth that now keeps her mouth open so she cannot bite down on her tongue anymore. We are so happy this has happened. The Attending PICU was actually talking about removing her teeth if they could not do something about it.
A close personal friend, Faith Miller, decides to come in from DeKalb and stay the night so she can visit with Mari and us. She is very close to Mari. She used to help me take care of her all the time. She has stayed at my house and gone on a trip with us before. Mari is like a sister to her at least if not like a daughter. She just loves her so much and was so excited when I invited her to stay the night. She and I stay at the Ronald McDonald House together. I have a decent night’s sleep. I only wake up once and then wake up right around 8am.
ab cd ab
I believe today is one of the best days for Mari in a while. It is a pretty uneventful day and that is what we are really hoping for as she does not need any more drama in her little life.
Faith and I come back to the hospital around 10am. Neurology has already come in by the time we make it there. They tell Keith that they want to do another CT scan tomorrow just to see how it has changed from her last one and also to check out the small bleeds they found in her brain from the MRI. They also want to repeat the MRI on Friday. I believe they want to do it then as that will be about 7 days from the time of her last serious injury. This will give them a good look as to the true extent of all her injuries in her brain. Sometime between now and Friday they also want another EEG performed as well. We are fine with all of that.
For the most part her stats seem to be pretty stable today. Her ICP (inter cranial pressure) seems to be getting higher and then staying in the 30s. This makes the neurosurgeons nervous so they want to have an immediate CT scan done instead of waiting until tomorrow morning. This is just as a precaution because no one wants what happened on Friday to happen again. So they immediately take her off of 24/7 dialysis and get her off to CT.
After they come back with her, the Attending comes in about an hour later to tell us what she thinks she saw. She says that her brain has been so injured the definition that would normally be there isn’t. There are two scenarios that the CT scan shows. The first one is that they have been draining way to much cerebral spinal fluid and the ICP is measuring the skull instead of the actual cranial pressure. The second one is that her brain is swelling again which is not good at all. I ask her what they would honestly do if it is swelling or if the small bleeds from before get bigger. She kind of hesitates at first but then says there is a procedure they really do not like to do but they can take off part of her skull until the brain quits swelling. However, she really feels it is the first one where they have just drained too much cerebral spinal fluid. She then looks over at the EVD, which is draining the cerebral spinal fluid from her brain, and notices that it has been changed from 10 to 20. She asks the nurse why it has been changed. The nurse says the neurosurgeon had called and told them to change it. She says this just confirms her assessment as the neurosurgeon also feels too much fluid has been being drained. We are all happy to hear that.
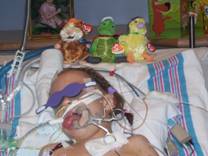 As
I sit here, her heart rate is sitting about the 130s and her blood
pressure is about 115/68.
She is doing pretty good.
In rounds this morning they decided to lower her respirations down to 15
and they have been there all day.
We are happy with that.
Her tongue is still very swollen but it is now pink and looks to
be a little smaller I think.
We are happy with where she is at tonight.
It is a pretty calm night.
As
I sit here, her heart rate is sitting about the 130s and her blood
pressure is about 115/68.
She is doing pretty good.
In rounds this morning they decided to lower her respirations down to 15
and they have been there all day.
We are happy with that.
Her tongue is still very swollen but it is now pink and looks to
be a little smaller I think.
We are happy with where she is at tonight.
It is a pretty calm night.
Keith heads over to the Ronald McDonald House around 8:30pm. Tonight should be a calm night.
ab cd ab
Well, this morning has started off in a really bad way. Mari’s ICP still has not gone down all night long. At 6:45 this morning, they decide they need another CT scan to check things out. Of course I am nervous as all get. I want to let Keith sleep as late as possible so I decide to call his mom to see if she thinks I should call him. She doesn’t know either. So I talk to his sister Amy and she says that I should go ahead and call him. Then I get to thinking that I should ask the PICU Fellow why the CT scan is needed. So, I have the nurse page the Fellow over so I can ask her. She comes over and tells me it is simply to find out if she is ok to start back up the CRRT (dialysis) machine again this morning. I feel so much relief after that. I am so thankful that is all it is for. So I decide not to call Keith as a result. They bring Mari back from CT. I ask what her ICP is and now it’s at 39 to 40. It has gone up a little from the night before but that is probably from them moving her around to do the scan. I call Keith at this point because I just feel so uneasy about everything. I just want to inform him of what has been going on. I tell him he can come over if he wants to but not that he has to. He says he is going to stay there and just get a little bit more sleep as he did not sleep very well last night. I say that was fine.
The Neurologist comes by for rounds around 8am and tells me that her CT scan is now worse than last night’s scan. They are going to be performing a couple of more tests to help us with the decision making process. I will tell you, I have never come to loath a phase before as much as I have “to help you with the decision making process.”
The first test is another EEG to check her brain waves and the second test is an ESG to check different parts of the brain for things. I just start to cry as soon as he begins talking to me about all of this. He also goes on to say that we are now back to where we were on Friday. I am plain flat crushed. I immediately call up Keith crying and ask him to come over to the hospital as I do not want to be alone. I just simply need him there. So he says he will be right there.
Keith gets to the hospital pretty quickly. Then the PICU Attending with all the Residents and Fellows come by to do their rounds for Mari. They talk about her CT scans and what their plans are for that day. The main thing Keith and I stress is to do nothing and just let her be stable for a few days. The doctor says that is exactly what the plan is. They are not going to reduce her ventilator as they have been the last couple of days to try to wean her off as she has not been doing very well having it done. Keith and I are fine with this.
They are first going to come in and do the EEG. They are in the process of setting it up when they decide to do the second test first. I watch the tech set Mari up. The tech first attaches to Mari’s wrists what is this blue like oval thing with contacts on it that kind of looks like what a 9 volt battery contacts look like. Then whatever she does with the machine, I watch Mari’s fingers kind of move and twitch. What is supposed to happen is the response from the fingers is then supposed to move up the arm, to the neck, through the spinal column, then through the brain stem, to finally reach the brain if everything is working correctly. The test takes about a half hour. They finally bring the tech back in for the EEG.
Around 10am, the Attending PICU says we are going to have another meeting sometime that afternoon to discuss what they have found. So I call up Keith’s mom to let her know. At first she does not want to tell Keith’s dad about the meeting because he has not been taking things well with what is going on with Mari. I tell her to let him make his own decision as to whether he wants to come or not. I do not want to hurt his feelings by not including him. Then Gina drives mom up to the hospital. Keith’s company commander Raina has also made it up to the hospital as well. She is such a support to us. We really appreciate her being here. Keith’s dad shows up first and then Keith’s mom and Gina.
I am having such a hard time by this point. You almost know what is going to happen. Ultimately, I decide I just need to get out of Mari’s room. So, mom, Gina, Raina, and I all go out to the PICU waiting room to just talk about anything but I think the obvious. It is hard for all of us. I think I am just completely numb. Keith finally comes in about 12:20pm to let us know that the meeting is scheduled for 12:30 in the small conference room.
We all leave the waiting room. I ask Raina if she will please go and stay with Mari so she will not have to be by herself while we are in the meeting. She says yes of course. Keith’s mom and dad, Gina, Keith and I all head over to the small conference room and wait outside the door. There are a couple of nurses in the room when we arrive as I believe this is the nurse’s lounge or something like that. Finally, Lori, the social worker, comes over and asks if the two women can leave for a little while as we are going to have a meeting in this room. They say certainly.
We all go into the room. They have to get more chairs for everyone. It is a big square table. We have Lori in there as well as Gretchen the PICU chaplain. I have formed a good bond with Gretchen and feel comfortable with her in there. Then the PICU Attending Melissa, the Neurologist Attending, plus all the Fellows and Residents that have been there that day working on Mari’s case, as well as Mari’s nurse.
Basically the meeting starts with the neurologist explaining how the ESG exam from that morning has turned out. What the test shows is that the charges stop at the brain stem and therefore never reach her brain. It never registered once that the test had been done. He then says that the EEG had minimal brain activity. They basically go onto tell us that Mari will never be herself again and we have forever lost our little angel. Our little girl we have grown to love. The one that was so full of energy and life. We have forever lost our precious baby girl and will never have her back again.
I start to cry and cannot believe what I am hearing. Even though, I think deep down inside I knew what they were going to tell us. Once I am somewhat able to calm down, we are able to ask if there have been any previous cases of someone like Mari that have ever recovered from something like this and they say no. I completely lose it. I break down like I did Friday when she went into cardiac arrest. I know right then and there I will never have her back. She is officially gone.
Now it is time to try to make a decision as to what we are going to do with Mari’s life. To describe what Keith and I had to go through this day, there are no words. How do you make a decision to permanently let your child go? To let them die when you know they are no longer the child you had before. How do you explain to your brain that just two weeks prior your child was running around, laughing, playing and just plain flat being Mari, our precious little angel, to now being completely gone spirit wise? To put it bluntly, you just can’t. It just doesn’t make any sense whatsoever.
Finally all the doctors and Mari’s nurse leave the room so we can discuss everything we have just heard. We ask Lori and Gretchen to stay. We all try to discuss what should be done because we do not want to be selfish and keep Mari here this way as she is already gone. She left the day she had her stroke. I actually wonder if her spirit left for heaven that day as well and is now in the presence of Jesus. At one point, just because of how the touchy the subject and situation is, I almost get into an argument with Keith’s dad. I think because he has a hard time hearing, he just does not understand everything we are saying. Keith and I kind of get into it as well over a couple of things because we are not communicating very well either. I guess you can say that this is the hardest thing that Keith and I are ever going to go through.
Ultimately we have Mom, Dad, and Gina leave the room so we can discuss what Keith and I are ultimately going to do. Then Lisa says we can talk to this nurse practitioner about things that can be done or questions we have. When Friday happened, Keith and I had made a decision that if Mari were to go into cardiac arrest again they could do chest compressions and they could give meds to help her but no shocking. We had also decided that if we were going to let her go that we would let her go via kidney failure.
Now we know we are going to let her go but we are not sure which direction is the best way to take. We ask the attending PICU doctor Melissa to come back in there so we can ask her more questions about how will be the best way to ultimately let her go. (It is still hard for me to think about how I have to voluntarily let her go. My mind just cannot wrap itself around this.) I feel like we are giving her the third degree and just grill her backward and forward trying to make our decision. I think some questions we may have even asked three or four times and decide to go a different route with the question each time to just really have all the information we need to make our final decision.
We talk about letting her go via kidney failure again but I know that we will want an open casket at the funeral. If she is to die of kidney failure then she will blow up like a big balloon and be so swollen. She will look nothing like herself after and I know I do not want that. Keith does not either. So then we ultimately decide to take her off of life support. We really grill the doctor about that. We want to know what will happen if she starts to breathe on her own. She says that there is a good possibility that she will have a brain hemorrhage. If she does not have a brain hemorrhage then she will probably die of kidney failure. We ask what will happen if she starts to breathe on her own, does not have a brain hemorrhage, and her kidneys start to work on their own. She says that they will no longer give her any fluids and take her off the feeds. Keith and I know we will not allow that to happen. It will be like we are starving her to death. There is just no way.
We finally tell the doctor that we want to take her off of life support that night. She leaves the room. Lisa then goes on to tell us about this photographer that gives of his time at the hospital and will take those last moment photos with you, your family and your child. I want that. I don’t know why. Keith does not but I do. I know I will not be able to look at them for a long time but I know I want them. The family all arrives during the afternoon. Even little Faith, our niece, who is 4 years old, comes up to the hospital. She had such a close relationship with Mari. Even though Mari really didn’t understand, Faith did. She loves our daughter so much. Mari is the closest to a sister I think Faith will ever have.
At this point, Keith, Grandpa, and Uncle Ruben go over to the Ronald McDonald house to pick up our stuff and check out of the room. While they are gone, I am able to give Mari her final bath. I wash her hair for what seems like forever, but probably only about 5 minutes. It is going to be my last time for everything and I just want it to last forever. I dry her body for the last time. I put lotion on her for the last time. I brush out her hair for the last time. I get her dressed for the last time. Her Aunt Amy helps me out. I paint her fingernails and toenails not only for the last time but also for the first time in her life as well (since she would never have sat still before for me to be able to do that LOL). I paint the fingernails on both hands and paint the toenails on her right foot. Then Aunt Amy comes back in the room and I ask her if she wants to paint her left foot toenails. She says yes. I don’t know exactly when Keith, Grandpa, and Uncle Ruben returned but they are there when it is time to do her hair. We decide to have it French braided like the nurse had done before. It is a total of 4 French braids. We sit her up and I hold her up for half of them. I notice that Uncle Ruben is just crying over to the side so then I ask him if he wants to help out and he says yes. So he sits their crying while holding her to get her hair braided. I try to share all of these last moments with everyone as this will literally be the last time any one of us will ever be able to do anything with her.
I think Keith’s company commander Raina leaves the hospital around 6pm. She has been such a good support for us. We let everyone have their last moments with Mari. We decide that we want everyone to leave the room about 7pm and just leave Keith and me to be alone with her.
During this whole time, the photographer has been taking pictures more in the background for all of our last moments together. When we have everyone leave, we keep the photographer in the room, Gretchen the chaplain, and of course the medical staff is there too. The nurse practitioner by this point cannot stay but did say good bye.
The doctor is ready to start taking Mari off the ventilator about 7:15pm. I get behind Mari and have her sitting up and leaning against me. I know there is no place else I could be. I have to hold my baby girl. She has been my life for almost 9 years. The doctor says it will be about a 5 minute process to take her off. She is at 17 reps per minute to begin with. About every 30 seconds it seems they put the reps down just a little bit further. I know when they finally take the tube out they have her down at 4 reps per minute. They finally take her off the ventilator and now we have to wait and see if she will breathe on her own.
I pick Mari up at this point and just hold her in my arms. She is my baby and I know I cannot just let her lay on the bed while we watch her pass in front of us. She starts this weird breathing. It is something Keith and I have never heard before. The best way to describe it is maybe someone with a really bad upper respiratory infection or maybe bronchitis. She does this about 4 to maybe 8 to 10 times a minute. I think about 5 minutes in the doctor does her first check to see if her heart is still beating and how strong it is. She says it is still going very strong. Before they started to take her off the ventilator, we asked about how long they thought it typically takes for someone to pass on and they said that every person is different but they would think about 20 to 30 minutes. Of course there are some that go quicker and there are some that last way longer. We just will have to wait and see.
I think I hold Mari for the first 5 to 10 minutes once she comes off the ventilator. Then I look at Keith and ask if he wants to hold her and he says yes. During this whole time, Keith and I are just sobbing. We know we are getting ready to permanently say good bye to our baby girl. We just love her and will miss her so much. At this point, we don’t even know just how much we will miss her we just know we will.
The breathing I described before we have been told is more or less a reflex and not her really breathing on her own. So basically it is just a matter of time. I know that Keith and I will never forget that sound as long as we live.
After about 5 minutes of Keith holding her in his arms I take Mari back in my arms. At first we are all sitting on the bed but my back starts to hurt so they bring over one of the bouncy chairs from the room and we moved to the chair. After 30 minutes have gone by, Mari is still with us and her heart is still beating quite strong. Mari has always been a fighter, even in the end. It is like she does not want to give up. It is like she is trying to have the last word. We keep talking to her and letting her know that it is ok to go. That we love her very much and we will miss her once she is gone but we will be ok in the end. During this whole time, Keith and I are just balling. We know how much we love her and do not want to let her go. We know that we are going to miss her so much.
I ask the doctor every so often to check her for her heart beat. Sometimes I can look down at her and I can see her carotid pulse (the pulse in your neck) beating away. I am secretly glad inside to still be able to see it. Toward the end, Keith and I are not really crying very much at this point. Keith keeps saying that he cannot go through this again. In other words, he cannot say good bye again if she holds on another day or two. It is just so hard on the two of us.
I just sit there rocking her while she is slowly slipping away from us forever. In those last 5 minutes or so, the doctor is finally telling us that her heart is starting to slow and is not as strong. We are relieved but so sad at the same time. I can still see her heart beating in her neck the last few times they have checked her. Then finally, the second to last time the doctor checks her, I can no longer see her pulse beating and she says that it is very slow. Then maybe 30 seconds to 1 minute later the doctor checks one final time and tells us that she is finally gone. She has finally succumbed to the disease that came so quickly just 2 weeks and 2 days before.
As soon as the doctor tells us that she is gone, Keith and I just break down hysterically crying as we know that we have lost her. It is just too unbelievable to comprehend. I hold her for a couple of more minutes and then ask Keith if he wants to hold her. He says yes. So I decide that I will go let the family know in the waiting room that she is gone. It is one of the slowest and loneliest walks I will ever take in my life. Imagine going to tell all of those who are waiting that the one person your life has been totally about for the last 8½ years is now just gone. We all walk back to her room together.
Once I arrive back in her room, I take her back in my arms for the next 20 minutes or so. I just sit there crying. Everyone else in the room packs up all of our belongings. I finally lay Mari down on the bed and just stand there in disbelief at what just happened. I am looking at Keith’s brother, his sisters and his brother-in-law all standing around Mari and talking. I don’t know exactly what they are talking about but they are just standing there. Then all of a sudden I become overly emotional again and just have to hold her one last time. By this point, the coloring has started to change for her. I guess it is from her being gone. I sit there for what seems like another 15 to 20 minutes just holding her, rocking her, missing her, and telling her how much I miss her.
I finally decide that I need to lay her back down in bed. This time I lay her in bed as if I am tucking her in for the night to go to sleep. I first lay her down. I gently put her head on her pillow. Then I take a blanket and cover her up. I make sure I put her arms on the outside and tuck her in all nice and tight. It will be the last time I will ever get to do that. I remember just looking at her and realizing how much I will truly miss her. That she is forever gone. We will never get to see that beautiful blue eyed, blond haired little girl run around. We will never get to hear her beautiful little sweet voice again. Just nothing.
I am just looking at her for the next several minutes. I do not want to leave that room. I am slowly walking out of the room just looking at her knowing that my life is going to forever be changed once I leave this room. I am walking out the room, around the partition that they had put up to give us privacy, and feeling so empty inside.
This is the story of what happened to our beautiful baby girl while she was in the hospital. Keith and I cannot say enough for how thankful we are for all the prayers and support we have received during this most difficult time in our life. There are no words to describe the true loss we feel but please keep us in your thoughts and prayers.
Love with all of our heart,Kristena and Keith
Mari’s mommy and daddy
Glossary
Plug Board